Is MonkeyPox Another Pandemic After COVID-19

Jennifer McQuiston, who works at the CDC headquarters as the deputy director of the high consequence pathogens and pathology division, said that monkeypox has symptoms similar to smallpox but are much less severe. Most people get better within a few weeks.
/cdn.vox-cdn.com/uploads/chorus_image/image/68568535/1230138068.0.jpg)
Since May 13, 2022, cases of monkeypox have been reported to WHO from three WHO regions and 12 Member States where monkeypox is not shared. Epidemiological investigations are still going on, but none of the reported cases has been linked to travel to endemic areas. Based on our current information, most patients have been found among men who have sex with other men (MSM) who go to primary care and sexual health clinics to get help.
This Disease Outbreak News aims to raise awareness, help with preparation and response, and give technical advice for actions that should be taken right away.
The situation is changing, and the WHO thinks that as surveillance grows in non-endemic countries, more cases of monkeypox will be found. Immediate steps are being taken to stop the spread of monkeypox by giving accurate information to people who may be most likely to get it. Based on what we know now, the people who are most likely to get monkeypox are in close contact with someone who had it while they were sick. WHO is also working to ensure that front-line health care workers and other health workers, such as cleaners, are safe. In the next few days, WHO will develop more technical suggestions.
Tells about the outbreak
As of 13:00 on May 21, 92 laboratory-confirmed cases and 28 suspected cases of monkeypox were reported to WHO from 12 Member States that do not have the monkeypox virus naturally. These cases came from three WHO regions (Table 1, Figure 1). So far, no deaths have been linked to it.
How the disease spreads
Monkeypox is a viral zoonosis which comes from animals and spreads to humans. It has symptoms very similar to those of smallpox, but it is less severe. It is caused by the monkeypox virus, which is in the family Poxviridae. In addition, it is in the genus orthopoxvirus. The West African clade and the Congo Basin (Central African) clade are the two groups of monkeypox virus. The virus was first found in monkeys in a Danish lab in 1958. This is where the name “monkeypox” comes from. In 1970, a child in the Democratic Republic of the Congo was the first person to be found with the virus.
The virus that causes monkeypox spreads from one person to another through close contact with sores, body fluids, respiratory droplets, and contaminated objects like bedding. The time it takes for monkeypox to spread is usually between 6 and 13 days, but it can be anywhere from 5 to 21 days.
Many kinds of animals can get sick from the monkeypox virus. The monkeypox virus’s natural history is still unclear, and more research is needed to find the same reservoir(s) and figure out how the virus keeps spreading in nature. One possible risk factor is eating meat and other animal products from infected animals that were not cooked well enough.
Monkeypox usually goes away on its own, but it can be awful for children, pregnant women, or people whose immune systems are weak because of other health problems. People who get sick from the West African clade seem to get less sick than those who get sick from the Congo Basin clade. Only 3.6% of West African clade cases end in death, while 10.6% of Congo Basin cases end in death.

Response from public health
In non-endemic countries where cases have been found, more public health investigations continue. These include finding more issues, tracking down their contacts, doing lab tests, treating patients, isolating them, and giving them supportive care.
When it was possible, genomic sequencing was used to determine which monkeypox virus clade(s) were involved in this outbreak.
Monkeypox vaccines, where they are available, are being used to protect close contacts, such as health workers. WHO is bringing together experts to talk about vaccination recommendations.
WHO has made surveillance case definitions for the current outbreak of monkeypox in countries where it is not commonly found.
Possible cause:
- A person of any age has an acute rash in a country where monkeypox is not shared.
Since March 15, 2022, you have had one or more of the following:
- Headache
- Fever that comes on quickly (>38.5oC), lymphadenopathy (swollen lymph nodes)
- Myalgia (muscle and body aches)
- Back pain
- Asthenia (a fragile feeling) AND
Varicella-zoster, herpes zoster, measles, Zika, dengue, chikungunya, herpes simplex, bacterial skin infections, disseminated gonococcus infection, primary or secondary syphilis, chancroid, lymphogranuloma venereum, granuloma inguinale, molluscum contagiosum, allergic reaction (for example, to plants), and any
Note that it is unnecessary to get negative lab results for the common causes of rash illness on the list for a case to be considered suspicious.
Benin, Cameroon, the Central African Republic, the Democratic Republic of the Congo, Gabon, Ghana (only found in animals), Côte d’Ivoire, Liberia, Nigeria, the Republic of the Congo, and Sierra Leone are all places where monkeypox is common. Benin and South Sudan have both shown that they used to import. Cameroon and Nigeria are the only places where cases of the West African clade are being reported right now. Using this case definition, all countries except these four should report new cases of monkeypox as part of the current multi-country outbreak.
Probable cause: A suspect is someone who fits the case definition.
Anyone or more of these:
Has an epidemiological link (face-to-face exposure, including health workers without eye and respiratory protection), direct physical contact with skin or skin lesions, including sexual contact, or contact with contaminated materials like clothing, bedding, or utensils to a probable or confirmed case of monkeypox in the 21 days before symptom onset. Has a travel history to a monkeypox endemic country1 in the 21 days before symptom onset.

The case is closed:
A case that fits the definition of a suspected or probable case and is confirmed in the lab to have monkeypox virus by finding unique sequences of viral DNA through real-time polymerase chain reaction (PCR) and sequencing.
The case was thrown out:
A suspected or likely case for which PCR and sequencing tests in the lab came back negative for the monkeypox virus.
WHO risk assessment
Monkeypox is a disease usually only found in West and Central Africa. In multiple countries, it is unusual to find confirmed or suspected cases of monkeypox without a history of travel to an endemic area. Because of this, it is essential to spread the word about monkeypox and do comprehensive case findings, isolation (with supportive care), contact tracing, and supportive care to stop the spread of the disease.
Cross-protective immunity from smallpox vaccination will only work for people over 40 or 50 since people under 40 or 50 no longer get protection from previous smallpox vaccination programs. People who are younger and live in countries where monkeypox has never been seen have little immunity to it.
In the past, people vaccinated against smallpox were less likely to get monkeypox. Unfortunately, although neither is widely available, a vaccine (MVA-BN) and a specific treatment (tecovirimat) for monkeypox were approved in 2019 and 2022.
Based on our current information, most cases have been found among men who have sex with other men (MSM) who go to primary care and sexual health clinics to get help. So far, there have been no deaths.
However, it’s not clear how far the disease has spread locally because there hasn’t been much monitoring. There is a good chance that more cases will be found with unknown chains of transmission, even in other groups of people. Since monkeypox has been found in several countries in several WHO regions, other countries will likely find cases.
The situation is changing, and the WHO thinks that as surveillance grows in non-endemic countries, more cases of monkeypox will be found. So far, this outbreak has not been linked to any deaths. Immediate actions focus on giving accurate information to people who are most likely to get monkeypox, stopping the disease from spreading further, and protecting people who work on the front lines.

WHO tells
It is likely that more cases will be found and that the spread will continue in the countries that are already reporting issues and in the other Member States. Therefore, any person who might have monkeypox should be checked out, and if they do have it, they should be kept away from other people until their sores have crusted, the scab has fallen off, and a new layer of skin has grown underneath.
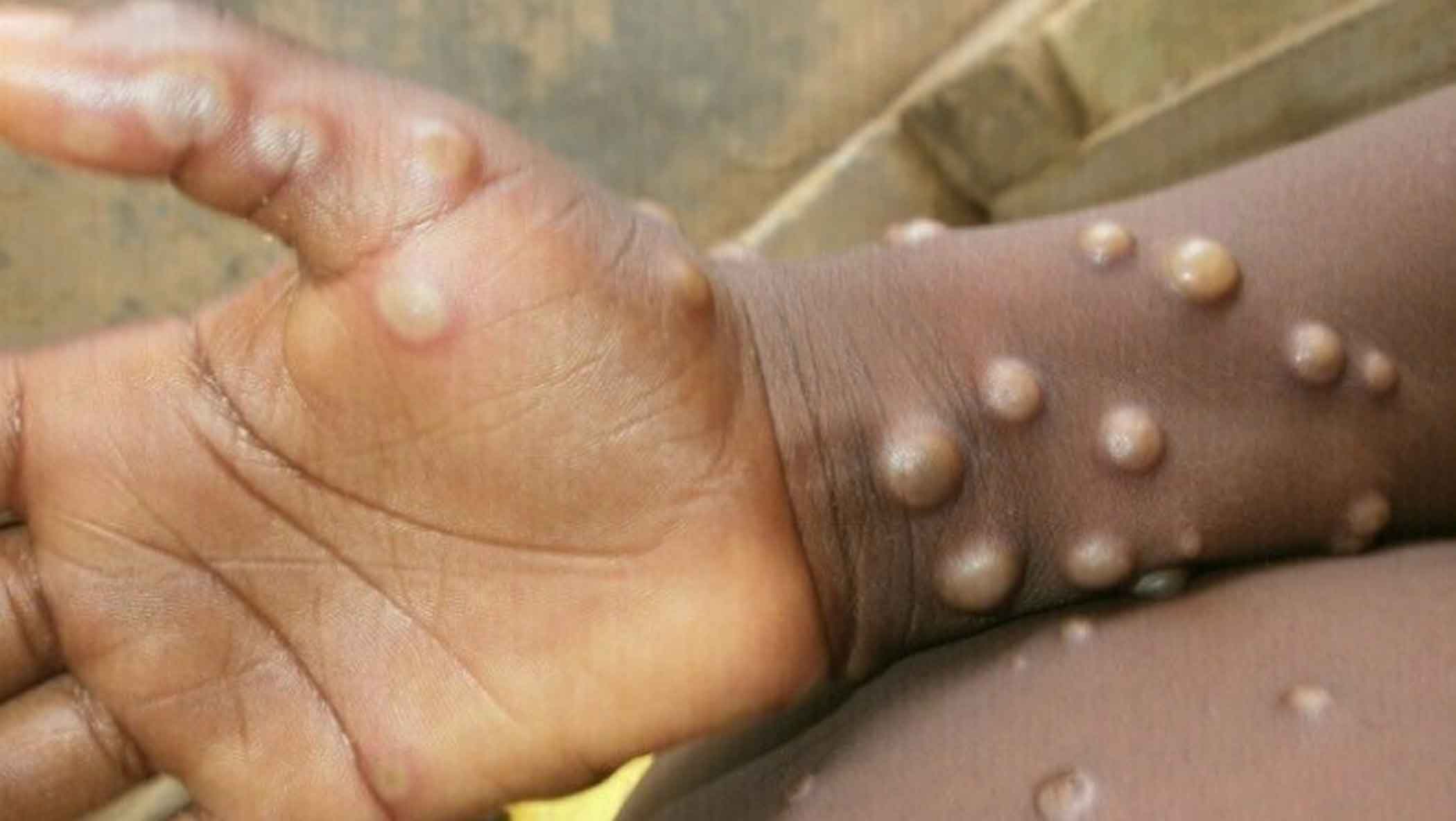
Countries should be on the lookout for signs that patients have an unusual rash that develops in stages: macules, papules, vesicles, pustules, and scabs at the same set of development on all parts of the body affected. This rash may be accompanied by fever, swollen lymph nodes, back pain, and muscle aches.
These people may go to a variety of community and health care settings, including but not limited to primary care, fever clinics, sexual health services, infectious disease units, obstetrics and gynaecology, urology, emergency rooms, and dermatology clinics. Therefore, it is essential to raise awareness in communities that could be affected and among health care providers and lab workers to find and stop secondary cases and effectively manage the current outbreak.
Things to think about surveillance and reporting
Surveillance
In the current situation, the main goals of surveillance and case investigation for monkeypox are to find cases, clusters, and sources of infection as quickly as possible so that the best clinical care can be given, issues can be isolated to stop the further spread, contacts can be found and managed, and effective control and prevention methods can be made based on the most common ways of transmission.
In places where the disease is not common, one case is considered an outbreak. Because a single point of monkeypox can be dangerous to public health, doctors should report suspected cases right away to national or local public health authorities, even if they are also looking into other possible diagnoses.
Patients should be notified right away, using the case definitions above or case definitions specific to a country. Under the International Health Regulations, both possible and confirmed cases should be reported right away to WHO through IHR National Focal Points (NFP) (IHR 2005).
Countries should be on the lookout for patients with an unusual rash, vesicular or pustular lesions, or lymphadenopathy, often accompanied by a fever. These symptoms can show up in various community and health care settings, such as primary care, fever clinics, sexual health services, infectious disease units, obstetrics and gynecology, and dermatology clinics. There should be more checks for illnesses that look like rashes, and people should be told how to get skin samples for testing.
Reporting
At the very least, case reports should include the following: date of information, reporting location, name, age, sex, and address of the case, date of first symptoms, recent travel history, recent exposure to a probable or confirmed case, relationship and nature of contact with probable or confirmed cases (if relevant), recent history of multiple or anonymous sexual partners, smallpox vaccination status, presence of rash, presence of other clinical signs or symptoms as per case definition, and date of confirmation (if done).
A form for reporting cases around the world is being made.
Things to think about when investigating a case
During human monkeypox outbreaks, the most critical risk factor for getting the virus is close physical contact with an infected person. If monkeypox is suspected, the investigation should include a clinical examination of the patient using appropriate infection prevention and control (IPC) measures, (ii) questions about possible sources of infection and the presence of similar disease in the patient’s community and among the patient’s contacts, and (iii) safe collection and shipment of specimens for monkeypox laboratory examination. Under “Reporting” above, you can see the minimum information that needs to be collected.
The investigation into exposure should look at the five to 21 days before symptoms start. Any person who might have monkeypox should be kept away from other people during the likely and known infectious stages of the illness, the pre-rash and rash stages, respectively. Even though lab confirmation of possible cases is essential, it shouldn’t hold up public health actions. More research should be done if there are signs of a similar disease in the patient’s community or among their contacts. This is called “backwards contact tracing.”
Cases from the past that were found through an active search may no longer have symptoms of monkeypox because they have recovered from the acute illness, but they may still have scars and other effects. Therefore, it is also essential to collect epidemiological information from past cases in addition to operational issues. Retroactive cases can’t be confirmed in the lab, but their serum can be taken and tested for anti-orthopoxvirus antibodies to help figure out what kind of case it is.
Samples taken from people who might have monkeypox or animals who might have been infected with the monkeypox virus should be handled safely by trained staff in well-equipped labs. During the packing of samples and the trip to the testing labs, national and international rules about transporting infectious substances should be strictly followed. To think about national laboratory testing capacity, careful planning is needed.
Clinical laboratories should be told when samples from people with suspected or confirmed monkeypox will be sent in. This way, the risk to laboratory workers can be kept to a minimum, and, when necessary, clinically essential tests can be done safely.
Things to think about when trying to find someone
Tracing people’s contacts is an essential public health measure to stop the spread of infectious disease pathogens like the monkeypox virus. It makes it possible to prevent the spread of disease and help people at a higher risk of getting a severe illness find out about their exposure more quickly.
This way, their health can be monitored, and they can get medical help faster if they start to feel sick. In the current situation, contact identification and contact tracing should begin as soon as a possible cause is found. Case patients should be talked to find out all of these people’s names and how to reach them. People should be told within 24 hours of being found.
What does contact mean?
A contact is someone who has had one or more of the following interactions with a probable or confirmed case of monkeypox between the time the source case’s first symptoms appeared, and all the scabs fell off:
meeting someone in person (including health care workers without appropriate PPE)
direct physical contact, including sexual contact; connection with contaminated materials, like clothing or bedding;
Contact identification
Cases can be asked to list contacts from home, work, school or nursery, sexual references, health care, places of worship, transportation, sports, social gatherings, or any other remembered interactions. Attendance lists, passenger manifests, and other things can also find people.
Keeping in touch
Contacts should be checked for signs and symptoms at least once a day for 21 days after their last contact with a patient or contaminated items during the infectious period. Worrying signs and symptoms include headaches, fever, chills, sore throat, malaise, fatigue, rash, and swollen lymph nodes. In addition, the temperatures of contacts should be checked twice a day. While the references are being watched for symptoms, they shouldn’t give blood, cells, tissue, organs, breast milk, or sperm.
Asymptomatic contacts can keep doing everyday things like going to work and school (they don’t need to be quarantined), but they should stay close to home for as long as surveillance continues. But it might be best to keep young children out of daycare, nursery, and other group settings.
The options for monitoring that public health officials have depend on their resources. Contacts can be watched in a passive, active, or direct way.
In passive monitoring, contacts are told what signs and symptoms to watch for, what activities are allowed, and how to contact the public health department if signs or symptoms appear.
Active monitoring is when public health workers check at least once a day to see if a person being watched has any of the signs or symptoms they have said they have.
Direct monitoring is a type of active monitoring that involves checking for signs of illness at least once a day through either a personal visit or a video check.
If a contact’s first signs or symptoms aren’t a rash, they should be kept away from other people and closely watched for a rash for the next seven days. If the contact doesn’t get a rash, they can go back to keeping an eye on their temperature for the rest of the 21 days. If the connection gets a rash, they should be kept away from other people, evaluated as a possible case, and a sample should be taken to test for monkeypox in a lab.
Keeping an eye on health workers and caregivers who were exposed
Anyone who has cared for a person with probable or confirmed monkeypox should be on the lookout for signs of monkeypox infection, especially in the 21 days after the last care. Health workers should let the authorities in charge of infection control, occupational health, and public health know about a medical evaluation to give them advice.
Health workers who have unprotected exposures (i.e., they aren’t wearing the right PPE) to patients with monkeypox or possibly contaminated materials don’t have to stay away from work if they don’t have any symptoms. However, they should be monitored for signs by taking their temperature at least twice a day for 21 days after the exposure. Before the health worker goes to work each day, they should be questioned about any of the above signs or symptoms.
Healthcare workers who have cared for monkeypox patients or had direct or indirect contact with them while following recommended IPC measures may have to do self-monitoring or active monitoring, depending on what the local public health authorities decide.
Some countries may think about giving people at a higher risk, like health workers and lab workers, a vaccination after being exposed (ideally within four days).
Finding people through travel
Officials in charge of public health should work with travel companies and their counterparts in other places to assess possible risks and get in touch with passengers and others who may have been in contact with an infectious patient while in transit.
Things to think about when talking about risks and getting the community involved
To stop the spread of monkeypox and get a handle on the current outbreak, it is essential to talk back and forth about the risks of monkeypox and involve communities at risk or have been affected in prevention, detection, and care.
This includes giving public health advice to the people who need it about how the disease spreads, its symptoms, how to avoid getting it, and what to do if an infection is suspected or confirmed. Together with this, community engagement should focus on the groups of people who are most at risk, working closely with health care providers, such as sexual health clinics and civil society groups.
Risk communication should be based on what you learn from social listening, which is a way to find out how people feel about something, and it should address any rumours or false information as soon as possible. For example, men who have sex with other men should not be judged because they have sex with other men. Instead, they should be given health information and advice (MSM).
Some important messages to prevent getting affected by Monkeypox
Prevention: Anyone who has direct contact with a person who has monkeypox, even if it’s sexual contact, can get it. Steps you can take to protect yourself include:
- Avoid skin-to-skin or face-to-face contact with sick people.
- Having safer sex.
- Keep your hands clean with water and soap or an alcohol-based hand rub.
- Use good breathing habits.
How to tell if someone has monkeypox and how to treat it: If someone has a rash, fever, or a sick feeling, they should see a doctor and get tested for it. If someone is thought to have monkeypox or has been confirmed to have it, they should stay away from sex, even oral sex, until the scabs fall off. During this time, patients can get treatment to help ease the symptoms of monkeypox. In addition, anyone who supports a sick person with monkeypox should take care of themselves by wearing a mask and cleaning things and surfaces that the sick person has touched.
Reporting: You should tell a doctor right away if you get a rash-like illness while travelling or when you get back. You should also say to the doctor where you’ve been, if you’ve been sexually active, and if you’ve been immunized against smallpox. In addition, residents and visitors of countries where monkeypox is common should stay away from sick mammals like rodents, marsupials, and non-human primates (alive or dead) that could be carrying the virus. They should also avoid eating or handling wild games (bushmeat).
Things to think about for large gatherings
Concerns have been raised in the media about how the monkeypox virus could spread more quickly at large gatherings. Unfortunately, large gatherings may be a good place for the monkeypox virus to apply because people are close, talk to each other for a long time, and talk to each other often. This can expose people to lesions, body fluids, respiratory droplets, and contaminated materials.
Even though researchers are still looking into how the current outbreak of monkeypox is spread, and they are likely different from how SARS-CoV-2 applies, it is essential to remember that the general precautions recommended against COVID-19 are also expected to protect against the spread of monkeypox virus.
Also, anyone who fits the above definitions of “suspected,” “probable,” and “confirmed” case should not get too close to other people and should not go to big gatherings.
WHO is keeping a close eye on the current outbreak of monkeypox. Even though there are no specific steps that need to be taken to hold, postpone, or cancel a large gathering in an area where monkeypox has been found, potential attendees can be given information to make an informed decision.
Things to think about when it comes to clinical management and preventing and controlling infections in health care settings
If a patient has suspected or confirmed monkeypox, health care workers should take standard, contact, and droplet precautions. These safety measures can be used in any health facility, from outpatient services to hospitals. Standard precautions include constantly washing your hands, taking care of dirty medical equipment, laundry, and trash properly, and cleaning and disinfecting surfaces in the environment.
Suspects or confirmed cases should be put in a single room with good ventilation, a dedicated bathroom, and staff as soon as possible. Cohort (confirmed with confirmed, suspected with suspected) can be used if there aren’t enough single rooms, but patients must be at least 1 meter apart.
Personal protective equipment (PPE) includes gloves, a gown, a medical mask, and goggles or a face shield to protect your eyes. If the person can handle it, they should also be told to wear a medical mask when they are close (less than 1m) to health workers or other patients. Lesions can also be covered with a bandage, a sheet, or a gown to make it less likely that someone will touch them. PPE should be thrown away before the patient is taken out of the isolation area.
Should aerosol-generating procedures (AGPs), such as aspiration or open suctioning of respiratory tract specimens, bronchoscopy, intubation, or cardiopulmonary resuscitation, be needed for any reason and cannot be put off, health care workers must use a respirator (FFP2 or EN certified equivalent or US NIOSH-certified N95) instead of a medical mask.
Isolation and precautions against spreading the disease should be kept until the symptoms go away (including the resolution of any rash and scabs that have fallen off and healed).
Antivirals like tecovirimat, which is approved for monkeypox but isn’t widely available yet, are one type of drug that could be used as a countermeasure. This is especially true for people with severe symptoms or at risk of having a bad outcome (such as those with immune suppression). A vaccine for monkeypox was just given the green light, but it is not yet widely available. Some countries might have smallpox vaccines that could be used in their national guidelines say so.
Depending on the land, any request for vaccine products may be available in small amounts through federal authorities. Countries might want to think about getting close contact, and certain groups of health care workers vaccinated right away as post-exposure protection or as pre-exposure protection for certain groups of health care workers.
Based on the available information right now, WHO does not recommend that the Member States take any measures related to international travel for both people coming into and leaving the country.
In the next few days, WHO will give some technical advice.
edited and proofread by nikita sharma




