Monkeypox virus: how deadly can it be? Experts answer the 3 most-asked questions and everything you should know about it.

Monkeypox virus: How deadly can it be? Experts answer the 3 most-asked questions and everything you should know about the virus, symptoms, risk factors, and prevention
HIGHLIGHTS:
Monkeypox disease, symptoms, and treatment
Occurrence of disease
Monkeypox cases have been reported to WHO in more than 3,400 different countries
Five Facts about monkeypox
Why India must be more watchful against Monkeypox
The Outcome of infection and risk in children
Therapeutics, vaccination, preparedness ,and response
What is Monkeypox virus?
The monkey virus, which causes smallpox, and the vaccinia virus, which was used in the smallpox vaccine, are also members of the genus orthopoxvirus, which also includes the virus that causes monkeypox. Compared to smallpox, monkeypox symptoms are less severe.
The smallpox virus was eradicated through vaccination in 1980, but monkeypox still exists in a large number of Central and West African nations and has occasionally been detected overseas. The Congo Basin clade, also known as the Central African clade, and the West African clade are two different clades, according to the World Health Organization (WHO).
A zoonosis, or illness that spreads from sick animals to people, is monkeypox. The WHO asserts these incidents frequently happen close to tropical rainforests where the virus-bearing animals live. Squirrels, dormice, rats taken from Gambian forests, and various kinds of monkeys have been found to be infected with the monkeypox virus.
However, there is a limited amount of human-to-human transmission. According to the WHO, the longest reported chain of transmission is six generations long, meaning the last individual to contract the illness in this chain was six links removed from the original ill person. Dr. Colin Brown, Director of Clinical and Emerging Infections at the UK Health Security Agency (UKHSA), stressed that monkeypox does not easily spread between people and that the overall risk to the general population is very low on Saturday.
According to the WHO, transmission can happen when people come into touch with bodily fluids, sores on the skin or internal mucosal surfaces, including the mouth or throat, respiratory droplets, or contaminated objects.
Monkeypox disease: Symptoms and treatment
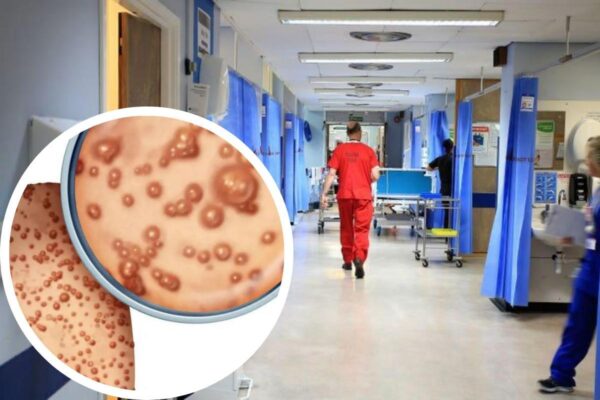
A fever, headache, muscle aches, backaches, and weariness are the first symptoms of monkeypox, according to the US Centers for Disease Control and Prevention (CDC). In contrast to smallpox, it results in lymphadenopathy, and swelling of the lymph nodes.
The WHO emphasizes the need to distinguish between monkeypox and other diseases like chickenpox, measles, bacterial skin infections, scabies, syphilis, and medication-related allergies.
It takes 7 to 14 days for monkeypox to incubate, but it can take up to 21 days. Within a day to three days of the start of the fever, the patient often develops a rash that starts on the face and spreads to other parts of the body.
The two to four-week skin eruption stage is characterized by the lesions becoming painful and hardening, filling with clear fluid and then pus, and eventually developing scabs or crusts.
The WHO asserts that the proportion of patients who pass away has ranged between 0 and 11% in cases that have been documented, and has been higher in infants and young children.
There is presently no effective, safe cure for monkeypox. The WHO offers supportive therapy based on symptoms. Awareness is crucial for the sickness to be managed and prevented.
Occurrence of disease
According to the CDC’s review of the disease, the term “monkeypox” was coined in 1958 after two outbreaks of a pox-like illness in colonies of monkeys held for research.
The first human case was documented in 1970 in the Democratic Republic of the Congo (DRC), at a time when smallpox eradication efforts were ramped up.
The WHO has received confirmed reports of monkeypox in people from 15 countries across four continents.
Locally acquired cases have been verified in the Democratic Republic of the Congo (DRC), Central African Republic, Republic of the Congo, Gabon, Cameroon, Nigeria, Côte d’Ivoire, Côte d’Ivoire, Liberia, and Sierra Leone. The DRC has the highest frequency of infection worldwide.
South Sudan and Benin in Africa, US, UK, Israel, and Singapore, have imported cases.
Monkeypox cases have been reported to WHO in more than 3,400 different countries:
The World Health Organization (WHO) reported more than 3,400 instances of monkeypox as of last Wednesday, with one related death. Most of these cases had their beginnings in Europe. According to a report issued by the WHO on Monday, 1,310 new cases, including cases of monkeypox, had been reported to the UN agency for health since June 17.
Even though it declined to declare monkeypox a public health emergency, the World Health Organization (WHO) acknowledged there were many unsolved questions surrounding the outbreak. The chief of the WHO declared that the threat posed by monkeypox had him “extremely concerned.” More than 50 countries have reported more than 4,100 verified cases thus far.
Five facts about monkeypox:
A big DNA virus in the orthopoxvirus family is monkeypox. The monkeypox virus, which is linked to smallpox but only affects humans, is present in some areas of Africa in rats and other animals.
Although orthopoxviruses don’t change much, the virus that is currently causing the outbreak has undergone a number of modifications.
In the US, at least two different strains have been circulating.
Monkeypox frequently manifests as a rash of blisters filled with fluid. People are infectious both during the rash’s duration and for two weeks after it disappears.
A previous smallpox vaccination offers 85% protection against monkeypox, according to experts reported by PTI.
Experts answer the 3 most-asked questions and everything you should know about the virus
Let’s have a look at these experts’ answers to the 3 most asked questions on monkeypox and how is it evolving and how far will it spread.
The monkeypox virus: is it evolving?
A big DNA virus in the orthopoxvirus family is monkeypox. The monkeypox virus, which is linked to smallpox but only affects humans, is present in some areas of Africa in rats and other animals. Orthopoxviruses are mutation-resistant, stable viruses.
Contrary to viral strains circulating in Africa, the virus causing the present outbreak has undergone a number of changes. A study from UNSW Sydney, as reported by the news agency PTI, explained that these changes may have an impact on how the virus spreads and how clinical disease manifests itself.
There have only been a few introductions, as there have been at least two unique strains in use in the US.
Whether the mutations have increased contagiousness or modified the clinical pattern to resemble a sexually transmitted sickness is still a mystery to experts.
Will these mutations change the ways it spreads?
Monkeypox is a respiratory virus that has never been linked to a sexually transmitted infection. However, the current transmission pattern is strange. There appears to be a very brief incubation period (about 24 hours) following sexual contact in some situations, but not all.
However, human-to-human transmission is solely to blame for the epidemic’s explosive rise in non-endemic countries in 2022. More cases than have been officially documented could exist.
According to the report, it is still unclear why the pattern has changed, if the virus has grown more contagious, or whether it is simply spread through personal contact, in particular, internationally connected social networks.
Will it spread far? Does COVID affect anything?
People with COVID have weakened immune systems as they recover. Therefore, COVID patients may be more vulnerable to other illnesses.
“With the measles infection, we observe the same. The immune system is weakened, and subsequent infections are more likely for two to three years, according to the report.
Why India must be more watchful against monkeypox?

In non-endemic nations, the greatest monkeypox outbreak in history began in May 2022. Although there haven’t been any cases of monkeypox reported in India since mid-June, given how quickly the disease is spreading in non-endemic nations, it is urgent that clinicians, public health experts, and policymakers have a better understanding of the disease’s epidemiology so they can be ready for anything.
Children, expectant mothers, and immunocompromised hosts are at particular risk of this disease and need to receive special care.
India and other low- and middle-income countries should take advantage of the monkeypox outbreak in non-endemic nations to improve public health surveillance and health system capacity for outbreak and epidemic planning and response.
The monkeypox virus (MPXV), a member of the Poxviridae family and the same genus as the smallpox virus, is the infectious zoonotic illness that causes monkeypox disease. It is a dsDNA virus, which is a double-stranded deoxyribonucleic acid. In 1958, the MPXV was found for the first time in a group of monkeys in a Danish laboratory.
During the continuous search for smallpox cases in the Democratic Republic of the Congo (formerly called Zaire) in 1970, the first human case was discovered in a nine-month-old baby. Since then, hundreds of instances of the disease have been documented annually in roughly 11 countries in Central and Western Africa. Though several animal species have been shown to be vulnerable to the monkeypox virus, it is still unknown what the virus’s natural host is. Further research is needed to find the reservoir(s) and understand how the virus circulates in nature.
In comparison to the high fatality rate of 30% for the smallpox virus, the case fatality rate for monkeypox is between 0 and 11%, which is slightly lower at 0 to 3% for the West African clade and 0 to 11% for the Central African (Congo basin) clade.
Human immunodeficiency virus/acquired immunodeficiency syndrome (HIV/AIDS) or other immunocompromised hosts have been the leading known causes of death in endemic countries up to this point, particularly in young children and immunocompromised individuals.
The extraordinary increase in infections during the current outbreak is due to the West African clade. As of June 15, 2022, 36 non-endemic countries had reported 2,039 laboratory-confirmed cases of monkeypox disease, according to the most recent WHO report.
Eighty-four percent of the cases were located in the WHO’s European area. However, there are reported examples involving imports, historical travel, and cases from the Americas, the Eastern Mediterranean, and the Western Pacific region. Among endemic nations, Nigeria has witnessed an increase in monkeypox cases since 2017.
The outcome of infection and risk in children
Monkeypox is often a self-limiting illness that stays mild, although it can become serious in children, pregnant women, comorbid people, and people with impaired immune systems. Miscarriages and fetal deaths have occurred as a result of monkeypox transmission through the placenta.
Uncertainty exists regarding the relationship between these outcomes and the severity of maternal sickness. The median age of monkeypox sickness in Africa has changed over time, going from four and five-year-old children in the 1970s and 1980s to 10 and 21-year-olds in the 2000s and 2010s.
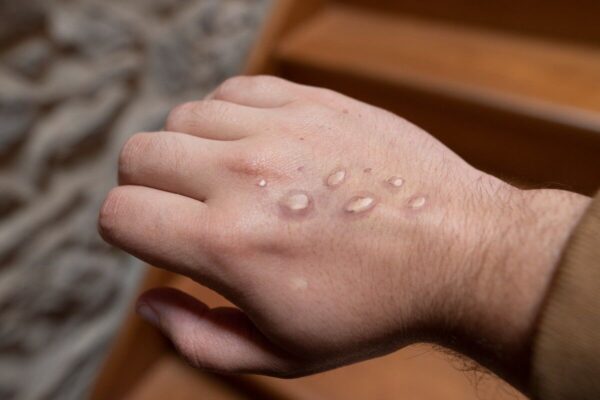
10 out of 34 (29%) of the confirmed patients during a previous outbreak in the US were under the age of 18. However, children made up about 8% of the 91 cases during the first year of the continuing outbreak in Nigeria, in 2017–2018.
According to a new longitudinal study from the Democratic Republic of the Congo, half of the 216 hospitalized monkeypox patients over the years 2007 to 2021 were children between the ages of 0 and 12.
Given the probability of negative outcomes in this demographic, the data available suggests that the risk of children having disease may have decreased over time. Nevertheless, children remain to be a more vulnerable group. The patient’s health status, the Congo Basin virus infection, the extent of virus exposure, and the type of sequelae all affect the prognosis.
Therapeutics
Monkeypox disease is typically controlled symptomatically, with complications managed and long-term consequences avoided. Fluid intake and proper diet are essential for enhancing overall recovery. Early in 2022, Tecovirimat, a medication initially investigated and created for smallpox, received approval for MPXV in a small number of nations; nonetheless, it is not yet generally accessible.
In animal trials, the effectiveness of two more antiviral medications, Cidofovir and Brincidofovir, which were also developed to treat smallpox and operate by preventing the viral DNA polymerase, was demonstrated. However, there is not enough information on their efficacy in treating human monkeypox disease.
Additionally, research on monoclonal antibody combinations is ongoing. The US Food and Drug Administration has authorized Vaccinia Immunoglobulins (VIG), which demonstrated some effectiveness against additional orthopoxviruses [35]. Further research is required, however, VIG contributes to post-exposure prophylaxis and lessens the severity of the sickness.
Vaccination
Observational studies have revealed that smallpox immunization can provide up to 85% cross-protection and can lessen the severity of monkeypox.
However, in the current outbreak, immunity from previous smallpox vaccinations may not be helpful because it is restricted to people who received the shot by or before the 1980s and because there is a good chance that the vaccine’s protective effect has already started to wane in that population over the past 40 years.
Since smallpox was eradicated in 1980, there are no public immunizations accessible. Given the lengthy incubation period, it is also thought that immunization, administered up to 14 days after exposure and four days before symptoms manifest, may help prevent sickness or lessen its severity.
In 2019, MVA-BN (Modified vaccinia Ankara -Bavarian Nordic strain), a third-generation smallpox vaccine, received approval to protect against monkeypox. This vaccine, which is believed to protect against MPXV, is based on a particular strain of the vaccinia virus. In numerous European nations, the United States, and Nigeria as of June 11, 2022, the MVA-BN smallpox vaccine is accessible, mostly for “off-label” use.

According to a provisional WHO recommendation, local authorities should think about utilizing authorized smallpox and/or monkeypox vaccines to combat the ongoing outbreak. For the ring vaccination in the monkeypox outbreak, only second-and third-generation smallpox immunizations, as decided and guided locally, may be used.
Non-replicating (MVN-BN) and minimally replicating (LC16) are preferable for women who are pregnant or nursing. MVA-BN and LC-16 are preferred for use with kids. Only LC16 has been licensed as vaccination for young children and newborns. MVA-BN, which is authorized for use in adults, can also be given to kids in a variety of circumstances as off-label use.
Preparedness and response
Every nation needs to be ready given the pattern of the spread. Priority should be given to outbreak readiness measures such as the establishment of designated isolation facilities with dedicated beds, the acquisition of tools and reagents for laboratory testing, and the education of a group of healthcare professionals to serve on a rapid reaction team (RRT).
The mainstays of the response continue to be early case detection, contact tracing, and, when and where practical, ring vaccination (of close contacts and family members).
Additionally, it must be kept in mind that although laboratory confirmation of suspected cases is required, public health measures shouldn’t be postponed. Similar to this, it is necessary to track down and conduct more research on patients and contacts in the area while waiting for the test confirmation (backward contact tracing).
Risk communication training should be provided to the relevant medical staff. When one or more MPXV cases are reported, extra effort should be put into educating the public about clinical symptoms and spreading preventive. It shouldn’t be overdone, either, as that can cause fear.
Guidelines for the diagnosis and treatment of monkeypox sickness have already been published by the Ministry of Health and Family Welfare (MoHFW). Intensified surveillance and early case detection utilizing established case criteria are prioritized. The nodal laboratory for monkeypox virus testing in India is a facility at the National Institute of Virology (NIV) in Pune.
The COVID-19 epidemic has increased the ability of several countries to do genome sequencing. Genomic sequencing would be helpful in the case of MPXV to pinpoint the clade and the chain of infection.
The repeated genomic sequencing, however, is of limited use because MPXV is a DNA virus with a sluggish rate of mutation.
Furthermore, the MPXV genome is six times larger than the severe acute respiratory syndrome coronavirus 2 (SARS CoV-2) genome at about 200,000 nucleotide bases, making genomic sequencing more difficult, time-consuming, and expensive, with only marginally more useful results.
Whether the MPXV can start a pandemic is a relevant question. There are a number of factors that make the pandemic spread of MPXV sickness unlikely. First of all, the virus has existed for 50 years and is not a new one.
The viral structure, transmission, and pathogenicity are reasonably understood. Second, the virus primarily causes moderate illness, as shown by the absence of any fatalities since the outbreak’s start.

In comparison to SARS-CoV-2, which had a respiratory spread and a large percentage of asymptomatic cases, it is less contagious and necessitates close human contact. A person is only contagious when they exhibit signs of monkeypox. Therefore, there is very little likelihood of transmission going undetected.
Fourth, a few smallpox vaccines are easily accessible, and their “off-label” usage can be advised. If necessary, global production can also be increased.
Fifth, it has a very low rate of mutation and is a relatively stable virus. Given this context, the majority of infectious disease experts are of the opinion that a monkeypox outbreak will not spread to become a pandemic.
The virus may currently be confined and a monkeypox outbreak efficiently controlled by quarantining contacts, isolating confirmed cases, and using approved smallpox vaccinations “off-label” for “ring vaccination.” At this time, immunization of the general populace is not advised.
The ongoing monkeypox outbreak also raises concerns about the coordination and reaction of a larger global public health community. Despite the disease being present in 11 African countries for more than 50 years, it is only now that high- and upper-middle-income countries are experiencing an outbreak that it is receiving international attention.
This reflects the bias that is inherently present in global public health, where diseases prevalent in low- and middle-income nations are not given the same priority for research and policy treatments. Discussion among experts at all levels on the technical aspects of the prospective application of smallpox vaccines in cases of monkeypox epidemics is necessary.
The national technical advisory group on immunization (NTAGI) in India, immunization working groups, and expert committees of the professional associations should discuss potential target groups and develop technical recommendations on potential target groups as well as plan, acquire, stockpile, and if necessary, deploy such vaccines.

Numerous viral and zoonotic diseases have first appeared in India in the past 20 years and then spread there again. Climate change is predicted to increase the risks of zoonotic infections and cross-species viral transmission.
Treatments for different illnesses frequently have similarities. Strong primary healthcare systems, efficient disease surveillance systems, a knowledgeable public health workforce, and an emphasis on the “One-health” approach—in which interventions are coordinated to protect the health of people, animals, and the ecosystem—are essential for preventing any such occurrence.
edited and proofread by nikita sharma




